New Zealand faces a major aged care bed shortfall, and retirement villages could help—if funding and policy barriers are removed. Enabling them offers a faster, cheaper solution than relying on public hospitals.
As New Zealand’s population ages, the pressure on our public health system continues o build. In a recent episode of The New Zealand Initiative podcast, Summerset CEO Scott Scoullar laid out a compelling case for why retirement village operators should play a bigger role in the solution — and what’s currently holding them back.
Below are eight key insights that stood out:
- Aged care is facing a massive bed shortfall — up to 8,000 more beds needed by 2030
- Operators are ready to help, but current funding models are holding them back
- Public hospitals aren’t designed for long-term care
- Aged care beds are significantly cheaper than public hospital beds
- Developing new aged care facilities takes time — and the clock is ticking
- Building consent reforms are a step forward, but more change is needed
- The retirement village sector can deliver — if enabled
- It’s time for serious dialogue between government and operators
- Let’s take a closer look at each of these key points.
1. Aged care is facing a massive bed shortfall — up to 8,000 more beds needed by 2030
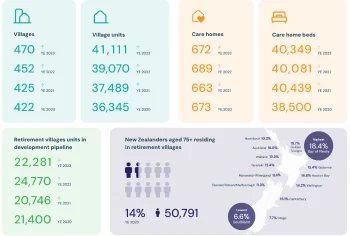
By 2030, there will be 130,000 more people over 85 in New Zealand. This means we’ll need about 13,000 additional aged care beds. The retirement village sector is expected to deliver around 5,000 of these beds, but that still leaves a shortfall of 7,000 to 8,000. If the government doesn’t act to build more facilities or help retirement village operators expand, the public health system will have to handle the shortfall.
2. Operators are ready to help, but current funding models are holding them back
Many of New Zealand’s largest retirement village operators are also major developers with the capacity to build more aged care beds. However, under current funding models, large-scale expansion is financially unviable. Without changes, operators are limited in how much they can contribute to easing the bed shortfall.
“We are here, we want to help, we’d like to build more care facilities — but the economics just don’t work.” — Scott Scoullar
“We are here, we want to help, we’d like to build more care facilities — but the economics just don’t work.” — Scott Scoullar
3. Public hospitals aren’t designed for long-term care
Older adults needing care often require support for extended periods — the average stay in an aged care facility is around 18 months. If they can’t access aged care beds, they’ll end up in public hospitals, which are not designed or resourced to provide long-term care.
4. Aged care beds are significantly cheaper than public hospital beds
According to Forsyth Barr’s 2024 report, government funding for a standard aged care bed ranges from approximately $175 to $300 per day, depending on the level of care. In contrast, a public hospital bed costs around $1,700 per day. Although aged care funding needs to increase, it would still be significantly less expensive than hospital stays.
5. Developing new aged care facilities takes time — the clock is ticking
New retirement villages (with attached aged care facilities) take years to develop. For example, it takes Summerset about three years from purchasing land to welcoming residents. Half of that time is spent securing land consent, with another six months navigating the building consent process. If new villages aren’t underway soon, New Zealand will face a serious shortage of aged care beds within a few years.
6. Building consent reforms are a step forward, but more change is needed
Recent changes allowing third-party providers to issue building consents are a positive step — Summerset has already partnered with one to speed up projects. However, further changes are needed to keep pace with the growing aged care bed shortfall.
7. The retirement village sector can deliver — if enabled
Retirement village operators are one of the largest public-private partnerships in New Zealand. With extensive experience and significant capital resources, they are uniquely positioned to expand aged care capacity. The missing piece is the right policy framework and support from the government. For the sector to deliver on its potential, policymakers must make growth possible.
8. It’s time for serious dialogue between government and operators
Retirement village operators need a seat at the table. They must be included in national conversations about aged care. It’s time to move past stop-gap solutions and engage in genuine, ongoing dialogue to unlock smarter, more cost-effective solutions that benefit all New Zealanders.
“We’re sitting here saying we’d like to be a part of that conversation… let’s have that rich dialogue.” — Scott Scoullar
“We’re sitting here saying we’d like to be a part of that conversation… let’s have that rich dialogue.” — Scott Scoullar
Final thoughts
New Zealand is facing urgent challenges when it comes to caring for its ageing population. It’s clear we can’t rely on the public health system alone. This interview with Scott Scoullar is full of honest reflections and practical ideas on how retirement village operators can be a bigger part of the solution. The entire episode is well worth a listen — you can find the full podcast here.